A pandemic of personal choice isn’t a pandemic you can overcome.
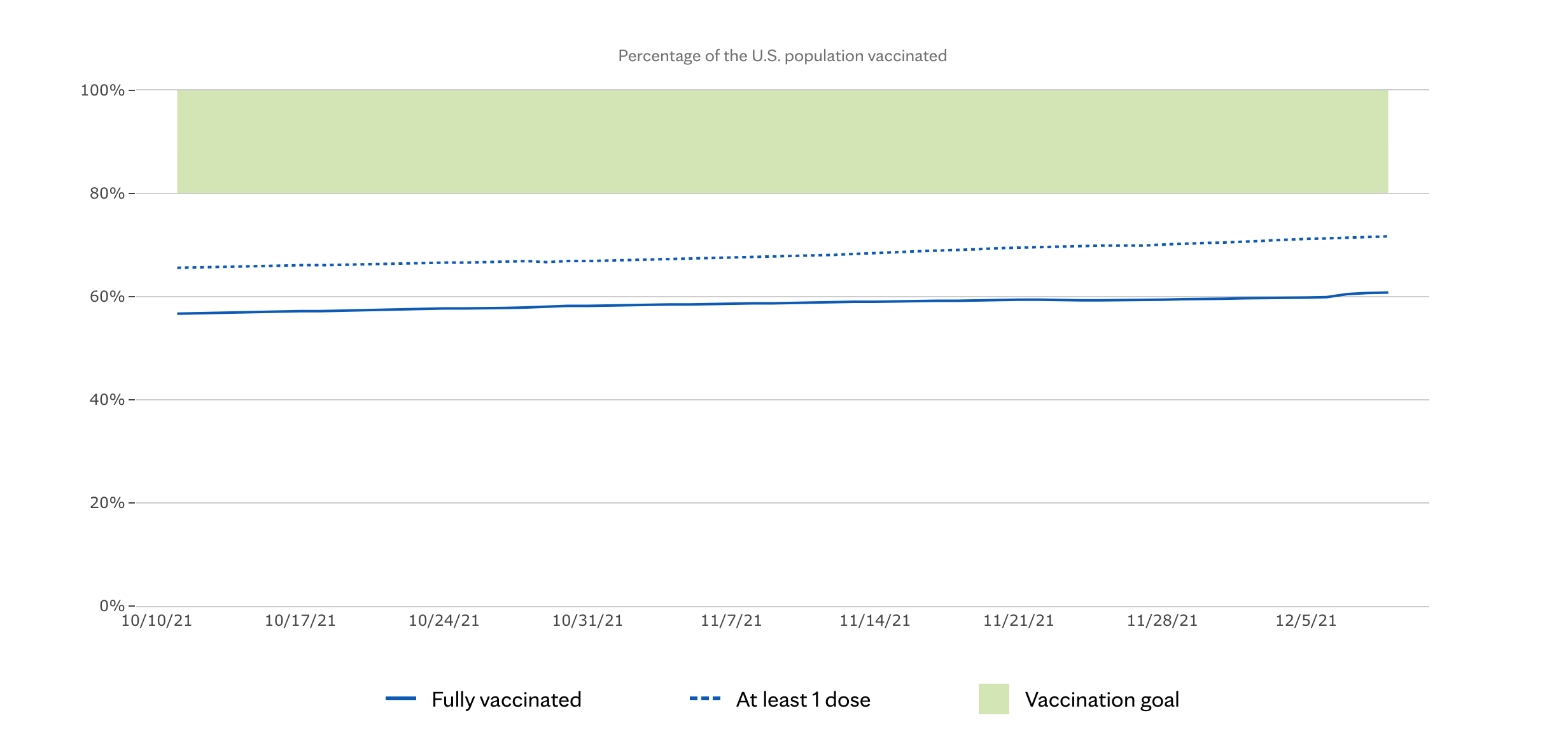
The last two-and-a-half years have been full of heartache and challenges. But with the ongoing vaccine rollout (children ages 5-12 just became eligible!) there’s growing hope that the U.S. will see the other side of this struggle soon. Despite vaccines being nearly ubiquitous across the country, roughly 30 percent of those eligible still have yet to get their first dose. With the volume of anti-vaxxers and protests against vaccine passports increasing, many vaccinated U.S. Americans are enraged at individuals who have yet to suck it up and get the shot. But many people who are unvaccinated are not anti-vaxxers, and directing our collective anger towards these individuals is misplaced.
***
Whose Burden Is It?
By constructing the pandemic as a fight between the vaccinated and the unvaccinated, we’ve removed the onus of healthcare protocol away from larger power structures
I, too, was enraged in the middle of last summer at people who refused to take such a simple step toward communal wellbeing. I wore my mask any time I was in public — outdoors or not — and I can count on one hand the number of times I left my parents’ house to socialize with friends from March 2020 through March 2021. My Twitter feed was a flood of my rants, cursing those who didn’t care about immunocompromised people like my sister and my mother who both have breast cancer. I was incensed at friends who asked me to hang out, forgetting tens of thousands of people, like my uncle and grandmother, died just a week before they were supposed to get the vaccine. “My body, my choice,” a phrase co-opted by the far right and anti-vaxxers, turned sour in my mouth. But it was in hearing the chants of these extremists that I began to unravel the numerous issues that come with letting individuals decide the fate of a community when such a catastrophic event has taken over the world.
In an August 2021 article published by the Los Angeles Times, Dr. Anita Sircar shares her firsthand frustration with unvaccinated people crowding the hospital emergency rooms and COVID units. And in her urging, she states that in such dire cases, “the burden of this pandemic now rests on the shoulders of the unvaccinated … the luxury of choice [does not exist].” And this is true; everyone should be getting vaccinated. But as we’ve seen throughout the pandemic (and human history), we cannot trust individuals to care about the community. Further, the burden has been misplaced. By constructing the pandemic as a fight between the vaccinated and the unvaccinated, we’ve removed the onus of healthcare protocol away from larger power structures that have the ability to create vaccine mandates.
The burden to remedy a global event shouldn’t rely on individuals. Not because individuals aren’t culpable, but because the only way to tackle global harm is with global policy.
The failure of government action was particularly evident with Donald Trump who turned the pandemic political. Just one of his many egregious blunders in office, his decisions to 1) refute the gravity of the pandemic, 2) refuse to implement policy and 3) suggest untested at-home COVID cures ensured that the fight against this SARS virus would be needlessly long and arduous. Countries like Singapore, New Zealand, Taiwan, and UAE were commended for their overall success, responding with aggressive nationwide lockdowns and/or contact tracing while also addressing their citizens’ needs so they were able to social distance. Those of us in the U.S. watched as these countries were allowed to resume their daily lives with minimal concern.
Though these nations need the vaccine to be fully safe, it’s important to remember vaccines are only one portion of the comprehensive plan — government action being another.
Failing Each Other
At nearly every juncture, the Biden administration has continued to prioritize the economy over people’s lives
President Biden and his team have done exceptionally little to mitigate this harm.
He has yet to release a national lockdown mandate as other nations have done and continue to do when their COVID numbers are as severe as the United States’.
The vaccine rollout plan functioned as a suggestion rather than firm protocol, and Biden’s office refused to send nations in the global south, namely India, the materials necessary to create the COVID vaccine even when those nations were at their worst. That allowed the virus to mutate and re-circulate the globe.
He allowed states to send students back to school in-person full time with few accountability structures in place. In many states this occurred around the same time the CDC suddenly said three feet of space was adequate for social distancing in the classroom. This is especially horrific considering that the majority of school-aged children at the time were not eligible for the vaccine yet.
Healthcare experts in the Biden administration did express concerns over the all-too-fast reopening of several states, but little was done legislatively to hinder or penalize state institutions and government officials who did not heed these warnings. At nearly every juncture, the Biden administration has continued to prioritize the economy over people’s lives until there is outcry from their center-left constituents.
Some suggest that those who choose to remain unvaccinated should face repercussions. Many of the suggestions are healthcare tariffs, but who does this really harm and who does it benefit? According to Daniel Polsky, economist and Professor of Public Health at Johns Hopkins, “Science and data are not sufficient to influence rational behavior.”
For the government to demand money in response to vaccine hesitancy or refusal would just be another form of corporal punishment that really affects only the poor. The wealthy, powerful moguls most efficient and prominent in disseminating anti-vax rhetoric are then left largely unpunished. The ever-circulating but unsourced quote “If the penalty for a crime is a fine, then the law exists only for the poor” seems particularly relevant here. In other cases, fines might do little other than increase resentment. Then there’s the issue of criminalization for which enforcement consistently and disproportionately harms Black and Brown people. Reinforcing oppressive harm structures to respond to social harm does little to progress towards a solution.
Further, when we place the onus on the unvaccinated to end the pandemic, we forget about the behaviors and practices of vaccinated people that also slow overall pandemic progress.
Vaccines were used by many as a free pass to behave as though the pandemic no longer existed. In April, Forbes reported a stark increase in international travel — particularly from the U.S. to other countries across the globe. Droves of people from the continental U.S. flocked to Hawaii as Governor Ige urged people to stay away, and Puerto Rico, despite its initial desire for tourists quickly repealed its marketing as tourists — vaccinated and unvaccinated alike — refused to follow basic safety measures.
The arrival of the vaccine meant many perceived the pandemic was over for them and therefore over for everyone. People — myself included at times — eagerly ripped off their masks forgetting that vaccination is not a cure but a safety measurement, a way to prevent hospitalizations and transmissions. I watched people shirk vaccine protocols, walking into coffee shops this past summer unmasked despite explicit signage, their vaccination status rendering them invincible and superior. While the best method to arriving on the other side of this pandemic, the vaccine is by no means the only practice which we should employ.
***
The Unvaccinated: People With Concerns, Not Agendas
When we peel back the layers of vaccine hesitancy, we see people who are concerned that the vaccine might not be safe, believe it was too rushed, or don’t believe it was tested on enough people. And despite all the tried and true science, hesitant people have the voice of anti-vaxxers and indifference chatting in their ears. Though we have comparisons — like the flu shot and every single vaccine children are required to get for school — this is the first time many of our peers are being confronted with the choice to get vaccinated. It’s also likely the first time, many people have thought to consider what goes into vaccines or have watched a vaccine be developed in real time. In these cases, throwing additional statistics in response to these concerns does little to abate them.
A method that has proven beneficial? Discussing the vaccine with primary care doctors. Not all unvaccinated people are staunchly opposed to the vaccine. The New England Journal of Medicine notes many unvaccinated people are “vaccine receptive” and “vaccine neutral” but are waiting for further encouragement from their primary care physicians or other clinicians within their community. For many, a familiar face or setting that can accompany them in getting the vaccine is the only push they need.
This observation is encouraging until we confront the U.S. healthcare system. Roughly 25 percent of American adults don’t have a primary care physician, and 15 percent are uninsured. These statistics are even more extreme in southern states and for populations of color.
From cost to time, the current healthcare model is inaccessible. If doctors’ offices — a core tenet of the healthcare system — are the most effective means for quelling vaccine hesitancy, where does this leave us as a nation as long as the state of COVID rests on the individual?
The unfortunate truth is that vaccinated individuals and healthcare professionals aren’t just competing against this monolithic anti-vax, anti-science mob. We’re also competing against misinformation, hearsay, and word of mouth from some well-meaning individuals being confronted with a health crisis for the very first time.
Fear mongering from news outlets and social media users alike isn’t helpful either. When researchers found that the Astra-Zeneca vaccine could be linked to recent blood clot cases, news outlets like CNBC headlined their articles “Blood clots linked to AstraZeneca shot have 22 percent mortality rate” rather than focusing on the fact only 4-6 out of every million shots would result in the condition. Similar occurred with the J&J vaccine. Then, there’s the more recent call for booster shots which has led some to wonder how effective the vaccines are at all, and if not, what the purpose is to get one now.
Though we have comparisons — like the flu shot and every single vaccine children are required to get for school — this is the first time many of our peers are being confronted with the choice to get vaccinated
I am hard-pressed to believe that you or someone you know has not used a “home remedy” or packets of Emergen-C to cure an ailment, or hasn’t used some hack that you’ve seen on the internet. While COVID is significantly more dire, for many, appealing to the statistical knowledge that vaccines work isn’t going to be productive if they have people in their ears saying “Hey, look at me! I don’t have the vaccine and I’m fine.”
It is understandable and all too easy to get angry at those who are unvaccinated. To see the long list of senseless deaths in this country and become enraged. To run out of compassion. But the individualist us-versus-them outlook only exacerbates the many other failures of the U.S. to engage with communal needs. It’s the answer to the question: why won’t people just get vaccinated if it helps others? It’s why states have rolled out an exhaustive list of incentives to get shots in people’s arms. At no point in history has individualism saved humanity, but it has continually been a central facet to community downfall.
Everyone should make the personal choice to be vaccinated, to do better for their community because it benefits everyone. But becoming irate towards a stranger who has just as many people telling them yes as they do telling them no isn’t going to quell the pandemic. Redirecting that energy towards public officials to create staunch mandates, increase access to healthcare, provide paid, guaranteed sick time for folks post-vaccination, be accountable for past and continued medical harm to marginalized folks, and to render the world virtually non-functional until individuals get vaccinated — these are long term solutions to an ongoing issue. While the U.S. has hopelessly fumbled the ball on COVID-19, this will not be anywhere near the last pandemic as worsening environmental factors enable the arousal of disease. What we can do is make sure we handle the next pandemic more efficiently and with community wellbeing at the forefront.
That’s a lot of words to use to be incorrect. Unvaccinated people are the burden. Pretending otherwise is intellectually dishonest.
How precious. How’re ya feeling? Any chest pains? Cancer? Is it time for your 7th boostie shot? lmao